Wednesday, March 15, 2023
Wednesday, September 7, 2022
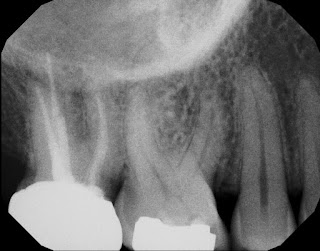
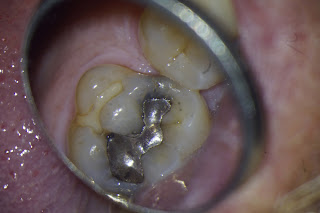
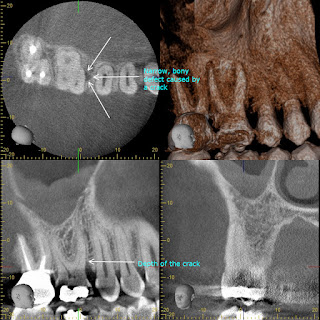
Using CBCT to Diagnose the Depth of a Cracked Tooth
One of the many uses of CBCT is to help us determine the depth of a crack - seen on the occlusal surface of a tooth, but uncertain as to how deep it goes down the root. Obviously the deeper the crack goes below the CEJ, the poorer the long term prognosis.
This patient was mostly asymptomatic until he recently bit into something and has had pain ever since.
Friday, March 4, 2022
Innovations in the Dental Insurance World
|
|
|
Monday, November 1, 2021
Survival in the Dental Office: Brain Based Leadership Concepts to Help your Practice
|
Monday, April 26, 2021
Dealing with Cracked and Fractured Teeth - An Inner Space Seminar
At a recent Inner Space Seminar, Dr. Jason J. Hales discussed dealing with cracked and fractured teeth.
Monday, March 8, 2021
Partner for Success - What Does A Real Partnership Look Like?
At Superstition Springs Endodontics, one of our five core values is "Partner for Success". To us this means, that we are successful when our partners are successful. As we have focused on this value, we have come to more clearly understand who our partners are, and how we can help each other be successful.
At SSE, our partnerships are primarily with our referring dentists, but also include other important providers of supplies, IT services, legal services, accounting services and even janitorial services. While insurance companies are often viewed as an adversary, we should look to build partnerships with them, when possible.
A 2009 study by the L.C. Williams & Associates Research Group details a group of dentists who refer less than 10% of their root canals to endodontists. This group of dentists have a very different perspective about working with endodontists. They tend to believe that they perform the same quality of endodontic treatment as specialists at a lower cost. They are less likely to admit that certain difficult cases should have been referred to an endodontist than their peers who refer more than 10% of their endodontic cases. These dentists are also less likely to describe an endodontist as their partner in delivering quality dental care. As you can imagine, these are not the dentists that we are interested in working with.
Defining this value of partnership has given us the freedom to realize that while most of our patients come from general dentists, there are times when we are forced to choose which dentists are given access and priority of our time, schedule and expertise. As you can imagine, those dentists with whom we have a partnership will get that priority. While working with this previously described group of dentists typically brings frustration, working in sync with partner dentists, and the relationship with them, is a rewarding and fulfilling part of our work.
- We will take care of their patients when in pain.
- We will stand behind the work we do for their patients.
- We will treat their patients the same way that they do.
- We will support their treatment plan.
- They can contact our doctors directly at anytime with any question or concern.
- Their patients will return more confident in their dentist and appreciative of their referral to SSE.
- We will do everything possible to help them be successful.
- Respect our team and their efforts to serve their patients
- Respect our time and are patient and flexible in getting their patients in
- They know our treatment is worth the cost. They encourage patients to see the value in coming to our practice regardless of insurance benefits or distance traveled.
- See us as a valuable part of their dental team - not just an emergency service or someone to call to bail them out when they get in over their head.
- See value in the work that we do for their patients. They recognize the expertise that comes with endodontic specialization.
- Are comfortable calling our doctors directly to help them deal with any especially difficult case or situation.
Monday, February 8, 2021
How to Manage Your Debt So It Doesn't Manage You
Tuesday, September 15, 2020
Aerosol Anxiety and COVID-19 Critical Thinking with Dr. Hessam Nowzari
- After 8 or 9 months, those who claim we don't have enough data for proper decision making are misguided or naive.
- Majority of current complications and deaths are based on decisions made upon flawed mathematical models.
- COVID-19 is not a novel virus. COVID-19 shares 90% of its genome with other coronaviruses - which we have been exposed to historically. We already have some amount of cellular immunity to COVID-19 because of our prior exposure to other coronaviruses. COVID-19 is an RNA virus which, by probability, gets weaker as it is replicated.
- The strength of the COVID-19 virus is the speed of contamination - not mortality rate.
- The US has ignored many of our scientific colleagues in Taiwan, Japan, Sweden etc. and the information and warnings they gave us early on and the success that they are currently having.
- We should expect to see increasing case positives and mortality rate as we move into October due to the regular flu season.
- We know that our young people are safe.
- We have to protect our elderly population and people with co-morbidities.
- COVID-19 is very sensitive to soap & water. Wash your hands with soap and don't touch your face or eyes. You don't need alcohol or expensive chemicals that destroy your natural biome.
- Every person has over 100,000 viral elements in their DNA. Viruses are part of who we are.
Friday, April 3, 2020
Your Brain and the COVID-19 Pandemic
Modern neuroscience has come a long way with the devlopment of the fMRI (functional Magnetic Resonance Imaging). This technology allows researchers to see the brain in action by visualizing the neural activity in real time.
David Rock, of the Neuroleadership Institute, coined the term neuroleadership to describe the application of the findings of modern neuroscience to leadership. This article will help you understand how your brain works and provide some tips to help you to better manage your own anxieties and negative emotions and better communicate, teach, train and mentor your team.
A Quick Summary:
The brain can be divided into the limbic system and the cortex.
The limbic brain is considered the primitive part of our brain because it is focused on survival. It is constantly scanning our world for threats and rewards. It the the emotional center of our brain and closely tied to memory. It has the ability to work at tremendous speeds and has inconceivable capacity. The limbic brain is the strongest part of our brain and will typically overpower/override our cortex. This part of your brain is causing you, and your team, to feel great anxiety in the current situation.
The cortex, and especially the prefrontal cortex (PFC) is the younger, conscious part of our brain. It is the center of conscious thought, reasoning, decision making, memorizing, inhibiting, recalling and moderating social behavior. The PFC is slower, limited in capacity and easily fatigued. While our cortex can easily be overpowered by the limbic brain, modern neuroscience shows that intentional or mindful use of our PFC can change the electrical activity of our brain. By consciously activating this part of your brain, you can inhibit some of the negative emotions and threats you and your team are currently feeling.
Your Brain During the COVID-19 Pandemic:
Right now, in the midst of the COVID-19 pandemic, your limbic brain is highly aroused and likely overpowering you prefrontal cortex, making it harder to make decisions and keeping you focused on the negative emotions and threats you are feeling. These threats include how to keep our teams employed, how to make rent, how to manage debt and cash flow, how to manage patient and employee concerns, how to interpret the laws that have been passed and applying and qualifying for loans with the CARE Act, just to name a few. Add to the fact that many employment lawyers and accountants are recommending layoffs or furlough for that team that you have worked with side by side for years. The 24 hour, non-stop media plays a huge role in activating a threat response in our brains to the current situation. Constant coronavirus headlines, drastic modeling predicting dire consequences make it worse day by day. Everything around you is stimulating the "fight or flight" reaction of the limbic brain. It's no wonder that we are all feeling threatened!
Overarousal of the limbic system overpowers and reduces the resources to the prefrontal cortex. This inhibits understanding, critical thinking, decision making, memorizing and inhibition, all of which you need to be the leader your practice. When the prefrontal cortex is overpowered, the we tend to do more "automatic" thinking and tend to respond more negatively to situations. We say things that we don't mean and that may trigger threats to the people around us. Because the limbic system is more affected by threats than rewards, you will find that threats to the limbic system come on faster, last longer and are harder to change. It becomes difficult to see the positive and we become more risk averse. We can only see the glass half full.
Neuroscience has shown that intentional use of the prefrontal cortex can change the electrical activity of the brain. The following techniques can be used to "put the brakes" on the negative emotions/anxieties that your limbic brain is currently focused on. These techniques can be helpful in every aspect of your life and help you as a leader.
- Symbolic Labeling: The act of consciously putting words to the emotions that you are feeling, expressed to yourself or others, actually stimulates the right ventrolateral prefrontal cortex (RVLPFC) which is the center of inhibition for your brain. This will help inhibit the negative emotions/anxiety that you are feeling due the powerful limbic response of your brain.
- Reappraisal: Reappraisal is another conscious activity of the prefrontal cortex which has been scientifically shown to inhibit the limbic response of the brain. Reappraisal is the conscious activity of looking at your situation from different perspectives. This requires more focus and energy, but has been shown to be more powerful than symbolic labeling at changing your brain's activity. Reappraisal can be done in the following ways:
- Reinterpreting: Consciously choose to reinterpret your current situation. Look for the positives and find opportunities in your situation. For example, "I have time to re-evaluation our systems" or "I have time to get more CE done" etc.
- Normalizing: Take a few minutes to focus upon what is normal about your situation. For example, "I am in the same boat as all the other dentists around me. We are all working through this together. etc."
- Reordering: Consider reordering what your values are in the situation. "My team or family's health is the most important thing right now." "I have to make this tough to decision to protect our practice so our team can have a job in the future."
- Healthy Brain Habits: Re-evaluate these habits in your life and prioritize them for better brain function.
- Sleep - get enough
- Nutrition - find balance
- Exercise - make time
- Breaks - time correctly
- Mindfulness Training - practice
Wednesday, April 1, 2020
Perspectives on the Pandemic - Interview of Dr. John Ioannidis of Stanford University
This is a follow up interview to his recently published article. I think you will find this a fair, balanced, rational and "science-first" approach to data surrounding the COVID-19 pandemic.