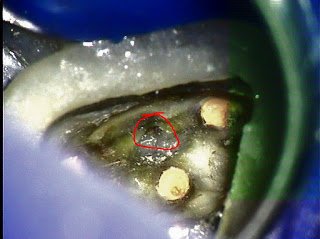
I realize that my last post was a little short. It was meant for the reader to contrast two root canal treatments on maxillary second molars and draw conclusions about differences. The obvious, and most important difference, is the treatment of 4 canals in the first case.
Here is the preoperative radiograph again:
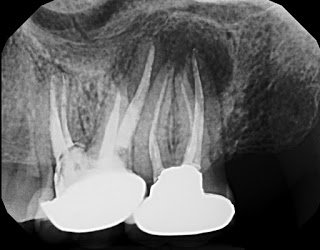
History: This patient has had symptoms on and off in the upper left for six years. She cannot chew comfortably on this side and feels a constant pressure in the area. She cannot walk up stairs without feeling dull pain in the area. The original treatment on #14 was performed in 2006 or 2007. Tooth #14 was then retreated by an endodontist in 2009, followed by persistent symptoms, and then treatment of tooth #15 soon after. With retreatment of #14 and treatment of #15, her symptoms improved for a short time, but soon returned.
Med History: Non-contributory.
Extraoral Exam: Alert/responsive, no extraoral swelling, significant asymmetry, or lymphadenopathy.
Intraoral Exam: All tissues normal in color and consistency, no swelling, no sinus tract, crown margins in tact. Large porcelain fracture on the occlusal of #15. All probing depths were 2-3mm with minimal signs of gingival inflammation.
Diagnostic tests: Tooth #15 was responded with a mild tenderness to percussion, both tooth #14 and tooth #15 were sore upon selective bite forces.
Radiographic Exam: Large radiolucency centered on #15 but overlapping the distal of #14. Widened PDL mesial #14. 3 canals obturated #15. Large, possibly strip perforated, canal preparation in the middle and cervical third of both #14 and #15, possibly compromising root strength.
The patient understandably harbored a very negative opinion of the success rate of root canal therapy. When patients harbor this attitude, treatment planning long, challenging retreatments with less than perfect success rates is usually out of the question. I recommended extraction of tooth #15, especially since saving the tooth would also require the investment of a new crown. I offered the alternative of a CBCT evaluation to aid in treatment planning any approach to saving the tooth. The patient understood my concerns, and opted for the CBCT. Here are some selected images from the CBCT.
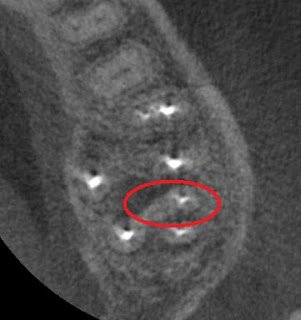
Circled is the MB root in cross section. From this view, it becomes apparent there is untreated canal anatomy in the form of a MB2 canal.
Even still, having looked through the CBCT images, I recommended extraction as the most predictable course due to the size of the lesion and the compromised tooth structure. The painted a pretty grim picture, but the patient asked me to take a chance on tooth #15 and consented to a guarded prognosis.
Following 2 hours of uninterrupted work at the first visit, where I had to fight to unledge all 3 previously treated canals, and was ultimately unsuccessful with the distal, calcium hydroxide was placed. The MB2 canal, while easy to see with the microscope, still consumed a majority of the time to navigate. The patient reported all symptoms resolved immediately following return of sensation, an unexpected result. She was able to run up stairs without pain that same night.
As you can see, still short on the distal where it was ledged. Some of the previous obturation in the palatal was unfortunately extruded. MTA was placed as a coronal seal in the cervical third and across the pulpal floor. Unknown to me at the time, she contacted her previous endodontist (in another city), who she still has a good relationship with to inform him of the outcome. She said he didn’t believe there was another canal in #15 and will likely be requesting CBCT and clinical images…I haven’t heard from him yet though.
It is unfortunate that so many patients I see have had unsuccessful experiences with dentistry and root canal therapy leading to negative opinions of the treatment options and profession. These patients are in our office literally every day, asking why? why? why? Here is another case of failure that required a consult lasting an hour and half to help the patient understand her condition, the etiology, and the treatment options (not many in this situation unfortunately). Having invested significant time and money in her teeth without success, it was challenging (understatement) to earn her trust in my diagnosis and plan.
#18 has a sinus tract tracing to the furcation radiolucency and a clinical class 2 furcation.
#19 has a narrow isolated 8+mm probing depth along the MB with an obvious apical-lateral lesion extending up the root.
For more case reports and content, please follow Alpharetta Endodontics on Facebook. www.facebook.com/alpharettaendo