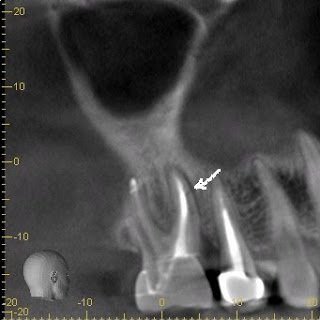
When we incorporated CBCT at Superstition Springs Endodontics, we hoped that it would be useful in identifying vertical root fractures. There is a significant learning curve with the use of CBCT and identifying vertical root fractures may be one of the most difficult things to interpret. The partnership with a good oral radiologist has also been an important part of learning to interpret CBCT.
In the past we have had to use clinical judgement, including presence of long, narrow periodontal pockets, j-shaped lesions as possible signs of vertical root fracture. However, those signs alone may also be caused by other conditions, not related to root fracture. Microscopic visualization was the most certain way to make this diagnosis. Too often, vertical root fracture is used as an excuse to remove a tooth without adequate evidence.
After more than two years of experience using high resolution, focus field CBCT in root fracture diagnosis, many consultations with the OMF Radiologist, we are more comfortable in diagnosing root fracture using CBCT, but the reality is that it is not always possible to see root fractures using CBCT.
Since the diagnosis of vertical root fracture (VRF) typically leads to extraction, it is our responsibility to be confident in that diagnosis. In order to definitely see a root fracture using CBCT, it seems the fracture has to open up to some degree. The more separation between fractured pieces, the better chance of making a definitive radiographic diagnosis. However, most vertical root fractures I see, do not have separated pieces.
Another challenge with identifying root fractures with CBCT is interpreting the difference between artifact (radiographic scatter) and actual fracture in the root.
Sometimes, a fracture cannot be seen with CBCT, but the bone loss pattern adjacent to a fracture can be seen. These bone loss patterns, not evident in traditional 2D imaging, can help identify the presence of a vertical root fracture. Even with CBCT, all information has to be evaluated and weighed and a judgment to be made. The only sure way is to see the fracture. CBCT does allow us to “see” the fracture in certain instances but not all.
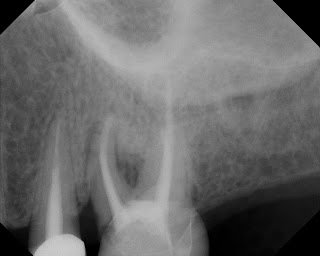
The following case would be typically diagnosed as a root fracture due to the bone loss pattern in the crestal area and into the furcation area as well as a long, narrow 8mm perio pocket on the ML surface. There is however, coronal leakage under the mesial margin which could be a source of re-contamination of the root
Rotation of the image, giving a palatal view of #14, shows a horizontal fracture in the MB root.
With these radiographic findings as well as the clinical findings, a confident diagnosis of vertical root fracture can be made. Extraction was recommended in