In cooperation with Dr. Tim Haegen of the Arizona Sinus Center, a division of Valley ENT, we have been able to help patients with chronic sinus issues. Many of these patients have bounced from ENT to ENT looking for answers, some have had continuous courses of antibiotics and some have had sinus surgery, only to continue to have chronic sinus issues. With some interdisciplinary education between endodontics and otolaryngology, familiarization with each other’s diagnostics and terminology and the use of medical and dental CT imaging, we are working together to diagnose and treat the often time overlooked odontogenic sources of sinusitis. The use of 3D imaging between disciplines has helped to bridge the gap of communication between medical and dental specialists trying to help patients with sinusitis and dental infections.
The following case demonstrates how proper understanding of endodontic and ENT imaging, diagnostics and terminology facilitate proper diagnosis and treatment.
This patient presented to Arizona Sinus Center for evaluation of chronic sinus issues. She presented with chronic, unilateral nasal and facial symptoms, along with foul smelling nasal discharge. Nasal endoscopy was performed and findings include:
FINDINGS:
- Nasal septum – superior deviation to right, mucosa intact, no perforation or crust
- Right inferior turbinate – normal
- Right middle turbinate – edematous
- Right middle meatus – closed; edematous medialized uncinate. Tissue is pulsatile. No purulence or polyps.
- Right posterior choanae – normal
- Left inferior turbinate – normal
- Left middle turbinate – normal
- Left middle meatus – open, no mucopus or polyps
- Left posterior choanae – normal
- Nasopharynx – no masses
- RADIOGRAPHIC FINDINGS:
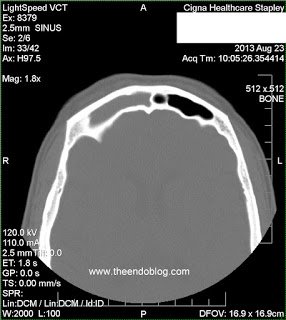
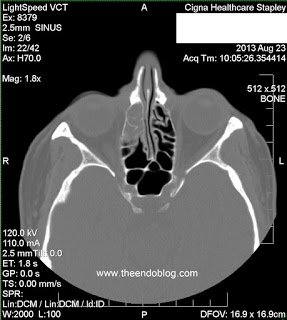
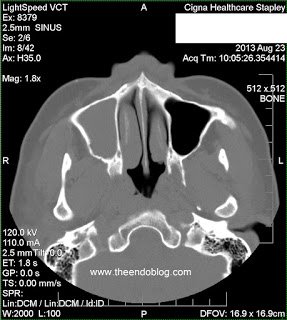
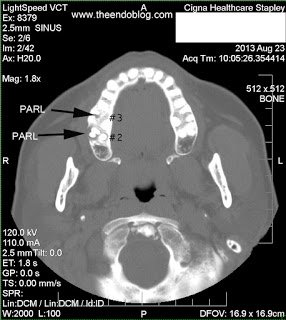
Following evaluation, the following impressions were recorded.
Impression:
- Nasal Obstruction
- Deviated nasal septum
- Frontal sinusitis, chronic
- Maxillary sinusitis, chronic
- Ethmoidal sinusitis, chronic
- Dental caries, unspecified
- Disturbances of sensation of smell and taste
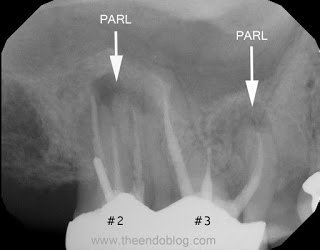
Endodontic diagnosis, including CBCT, determines that tooth #2 has a prior root canal with a root fracture and extraction is recommended. Tooth #3 has a prior RCT with apical abscess – caused by a missed MB#2 canal during the initial root canal treatment. Retreatment of the root canal #3 is recommended.
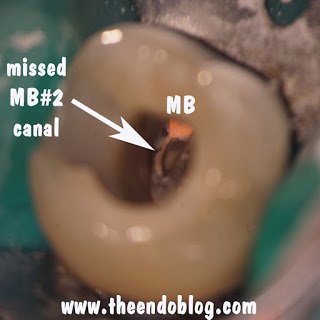
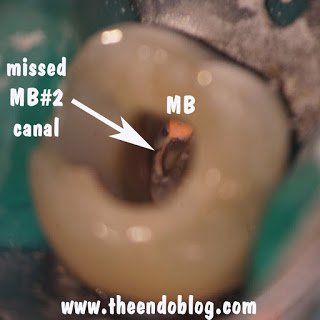
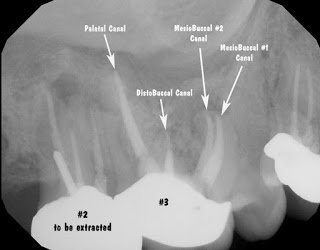
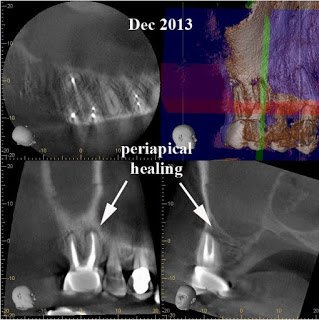
After 6 months, extraction of tooth #2 and retreatment of tooth #3 has shown periapical healing. The potential odontogenic source of the sinus infection has been eliminated. Since the Mx sinus continues to show opacification, the patient is referred back to Dr. Haegen for continued sinus evaluation and treatment.
Why See An Endodontist?

The endodontists at Superstition Springs Endodontics are experts in endodontic diagnosis and have extensive experience with CBCT. In addition, endodontists are specially trained to perform the most difficult endodontic cases. Maxillary molars, most closely associated with the maxillary sinus, almost always have 4 canals.
A common reason for root canal failure on Mx molars is inadequte cleaning, and often completely missing the MB#2 canal. Endodontists using an operating microscope are able to find and treat the MB#2 (4th canal) more effectively and efficiently. Endodontist are also trained to perform endodontic microsurgery when traditional endodontic therapy is unsuccessful.
When endodontists and otolaryngologists work together, they can provide the best care for patients with odontogenic sinusitis.

