Dr. Hale’s excellent post on pulp canal obliteration inspired me to share these few cases where a coronal barrier was also used to avoid root canal therapy. The most recognized reason to avoid complete pulpal debridement is biological, to maintain pulpal vitality, and thus continue root formation, subsequently improving fracture resistance, but there also exist technical limitations on the debridement procedure, imposed by anatomy or resorptive defects, that might prevent success of conventional root canal therapy.
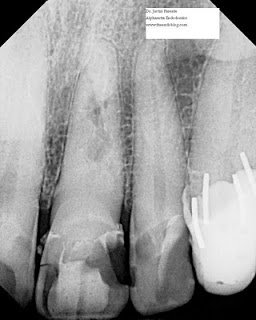
This first example is a straightforward partial pulpotomy (or Cvek pulpotomy) with an MTA direct pulp cap. This patient had cerebral palsy and toppled out of his wheel chair causing a complicated (pulpal involvement) crown fracture of #10. You will note #9 was treated at this time as well, and if I recall correctly, was discolored and non-vital from a previous similar trauma. Multiple dental injuries (and traumatic injuries of all kinds) are very common in CP patients due to negative effects on balance. Fortunately, working with a pediatric dentist who scheduled OR time, the patient was seen within two days of the incident and the pulp vitality of #10 was maintained. Remember, inflammation in traumatic exposures very slowly spreads apically, and immature pulps with large vascular supplies are largely resistant to necrosis in the short term.
At a 1 year recall, #10 responded normally to vitality testing. Radiographs revealed a complete formed root and a dentin barrier beneath the MTA. Astute viewers will note this success is amazingly in the absence of a coronal restoration (unfortunately, not the only time I’ve seen bare, unrestored MTA pulp caps succeed at 1 year recalls).
This next case is similar, although a little less conventional. As you can see in the preoperative radiograph, the root is severely dilacerated. While certainly it is possible to perform root canal therapy on this type of root (see my previous post for an arguably more challenging S curve), the difficulty level is unquestionably high. This treatment plan not only reduces the risk of instrument separation, but also saves the patient time and money, and the operator from fatigue.
The key here is that this was an asymptomatic carious pulp exposure. In the case of symptoms of irreversible pulpitis, it is generally thought that an MTA pulpotomy is a more risky procedure. It is certainly contraindicated in cases with symptomatic apical periodontitis (although I have had success direct pulp capping an immature tooth with apical periodontitis).
This last case is open to the most controversy. This patient had multiple large composite restorations across the anterior maxillary dentition. He admitted to being far more motivated by financials than esthetics. His previous composite restoration and crown had sheered off unconventionally at an oblique angle to the buccal leaving a substantial cingulum. The fractured portion had been rebonded by his general dentist. This tooth had a history of trauma over 40 years ago and some extensive external resorption is visible overlapping an obliterated pulp chamber and canal. The PDL is definitely in tact and there is no history of symptoms. The option of extraction and implant placement was discussed and encouraged. The alternative treatment plan chosen by the patient is less than ideal and the patient was more than okay with a compromised long-term prognosis. I intentionally described a grim outlook to the patient, as I do with most unconventional treatments, although here I can admit that I am confident in the predictability of the patient’s choice. As you can see from the preop radiographs, conventional root canal therapy is impossible due to the irregular resorptive defect sandwiched between obliterated canal space.
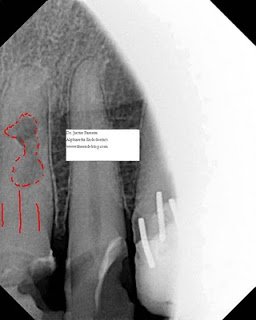
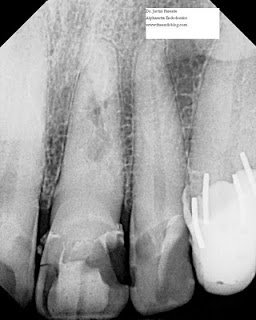
I am still waiting on the general dentist to forward over a restored recall radiograph. Hopefully I will have the image to edit in by the end of the week. You can see the post space that I prepared using a 2 round bur and a gates-glidden with the tip flattened. The post space communicated with the resorptive more coronal than I anticipated, necessitating the use of MTA as a sort of resorptive cap. I feel as long as the area remains aseptic, it is reasonable to assume a successful result.
Here is a bonus case posted on our facebook page, http://www.facebook.com/pages/Alpharetta-Endodontics/137382942943581 . I’d encourage everyone to follow there (and check the backlog of case photos) for more interesting cases.
The patient’s symptoms were intermittent, spontaneous, a 6 or 7 out of 10 on the pain scale, occasionally throbbing, and worse with mastication and pressure. The key history here is the patient’s remark, “it feels like my gums are coming loose from my tooth.”