In case you are a new reader, it merits repeating that the dental operating microscope is the most valuable tool available for providing endodontic care. The light and magnification provided are critical to success. With this post, I will present two recent cases where two different clinicians had difficulty locating canal anatomy and perforated the root structure. Each case was originally treated by a general dentist within the last year or two. With the use of a dental operating microscope, I was able to locate the missed canals and repair the perforations. Hopefully, our clinician readers who are not microscope trained will become motivated to invest in one.
Case 1
This patient described an on and off awareness of her tooth since root canal treatment by her general dentist. Her symptoms began to worsen, and she noticed a bump on the gums that drained. Her general dentist had admitted to difficulty locating a challenging ML canal.
There was no clinical sign of swelling or of a sinus tract at our appointment. The tooth was tender to percussion and uncomfortable to palpation in the furcation area. Probing depths were 2-3mm with some bleeding and serous drainage on probing in the furcation area on the buccal.
A diagnosis of previous root canal treatment with a chronic furcation abscess was made. I discussed the findings and treatment options at length with the patient. When a perforation exists for a long time and then becomes infected, our success rate with retreatment drops by some indeterminate margin, and the treatment was not without risk. The patient opted to take a chance on saving her tooth.
Upon access, purulent drainage was found pushing up from the gutta percha in ML area.
After two weeks of calcium hydroxide treatment, the patient returned symptom free and with improvement in the periodontal health. You can see on our post op radiographs just how large the perforation was.
At a follow up visit, the patient remained symptom free and the periodontal health continued to look good. The extruded MTA does not appear to have affected the outcome, which is consistent with the findings of others. For example, see this case of a large furcation perforation repair by Dr. Hales: http://www.theendoblog.com/2008/06/herodontics.html
Case 2
This patient initially presented with a chief complaint of minor soreness to bite forces and an intermittent dull pressure ache that she described as emanating from between the teeth #13 and #14. Her symptoms were described as unchanged with root canal treatment by her general dentist within the last six months. She described an improvement in symptoms when flossing and flushing between her teeth with Peridex.
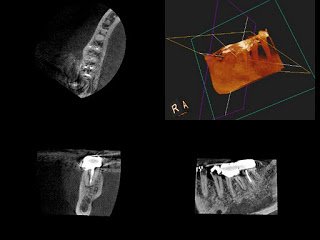
The tooth was slightly tender to bite forces and percussion, but there was again no signs of swelling or a sinus tract. The probing depths were 2-3mm with a 7mm pocket on the MB and a 6mm pocket on the DB. Because of the bilateral probing and bone loss, and the symptoms unchanged with root canal treatment, I recommended a periodontal evaluation. I knew that there was an untreated MB2, but the periodontal symptoms did not match up. After periodontal treatment, the pocket on the distal resolved, and there was a short-term improvement in symptoms, but they soon returned. At this point, I was suspicious of a perforation. A CBCT would certainly help confirm the diagnosis and be of value, but a decision was made to access and investigate.
At the first visit, the patient was made aware of a fracture from the mesial to the distal that dramatically decreased the prognosis for the tooth. After the first visit, the patient’s symptoms resolved, and she could chew comfortably. A case could be made to have the tooth immediately extracted, but the patient opted to finish the treatment even with the uncertainty involved.
In each of these cases, it is clear from the preoperative radiographs, that the clinicians who originally treated these teeth had good command over the processes of instrumentation and obturation. Both cases are instrumented to length (with the exception of the DB of #14), and appear well obturated with Thermafil carriers. Both clinicians were aware of the missed anatomy, but could not locate the ML and MB2 canals respectively. They were certainly difficult ones to find; they were not immediately obvious upon access, and while I do have extra training in endodontics, the microscope is what enabled these teeth to be saved. The long-term prognosis of either tooth is not great, especially the fractured #14, which could fail in the short-term, but the patient’s were well educated and appreciate the risks involved. The patient with tooth #14 is now prepared for the eventuality of a dental implant in that site.
The success of perforation repairs depends on many factors, such as the time since perforation, the location within in the tooth, the size of the perforation, and the materials used for repair. The smaller and more recent the perforation, the better the chance of success. The farther apical the perforation, the generally better success with repair, as long as the true canal path can be recaptured. Furcation perforations are the easiest to access for repair, and have the best surrounding tooth structure. Perforations in the gingival attachment level have a decreased prognosis due to difficulty controlling materials and the increased risk of a periodontal defect. In the Toronto studies (Friedman 2004), a prospective longitudinal study of the success of endodontic retreatment, of the 8 cases, roughly half of the retreatments with perforation exhibited healing. However, the materials used for repair in this this study were glass ionomers. In another study, 16 out of 16 cases repaired with MTA exhibited healing at a minimum of 1 year (Torabinejad 2004).
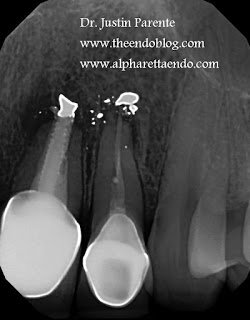
All three teeth in this posted here I consider to have guarded long-term prognosis. However, all three patients continue to chew and function in the absence of disease. If you have any questions or input, please let us know.
Any suggestions for future topics or posts are also welcome!